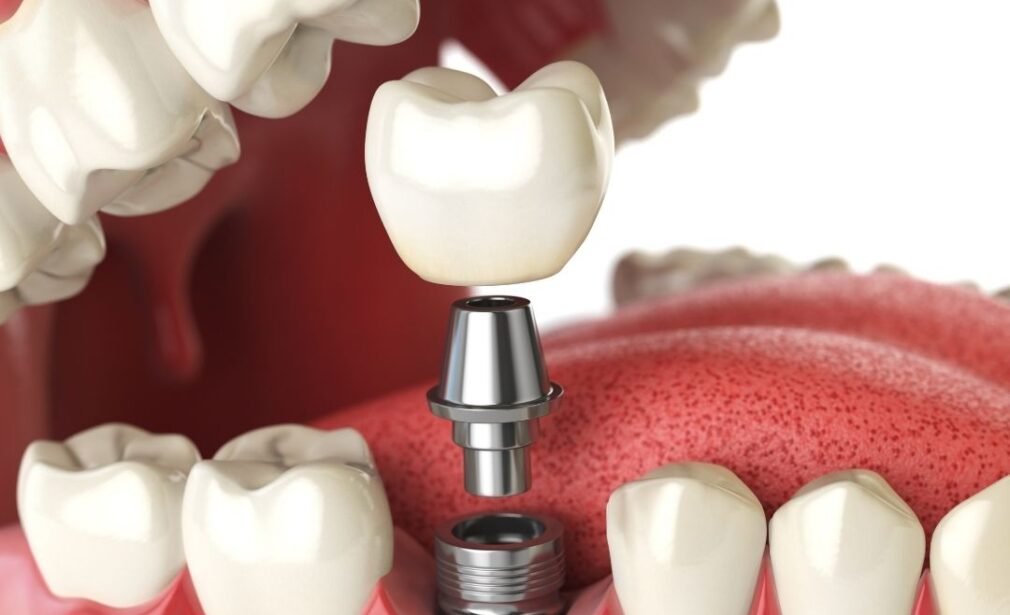
Implant Treatment (Dental Implants)
Information Page for Istanbul Bağcılar Yüzyıl Mahallesi and Surroundings
Implant treatment is a dental procedure in which titanium or titanium alloy artificial roots are placed in the jawbone to replace missing teeth. Dental implants provide an infrastructure that allows prosthetic teeth to be built on it by attaching to the bone similar to the natural tooth root. This page provides comprehensive information about what implant treatment is, what stages it consists of, for whom it can be considered and for whom there may be limitations, and the maintenance process.
Note In accordance with the current legislation on promotional and informational activities in health services, this content may only be used for information purposes has been prepared. It does not constitute a promise of treatment, guidance or advertising. Suitability for implant treatment is evaluated only after individual dental examination and necessary examinations.

What is a Dental Implant?
A dental implant is an artificial root system, usually made of titanium, that is placed into the jawbone in the area where the missing tooth is located. The implant itself is not a “tooth” on its own; together with the prosthesis (crown, bridge or prosthetic fasteners) placed on it, it helps to complete the missing tooth functionally and aesthetically.
Since titanium is a material that has a high biological compatibility with body tissues, it can be used as an implant between the implant and the jawbone over time. osseointegration a process called fusion can take place. At the end of this process, the implant transforms into a stable support structure capable of bearing the masticatory forces. However, this may not happen at the same speed and level in every patient; factors such as bone quantity, density and systemic health status are important in treatment planning.
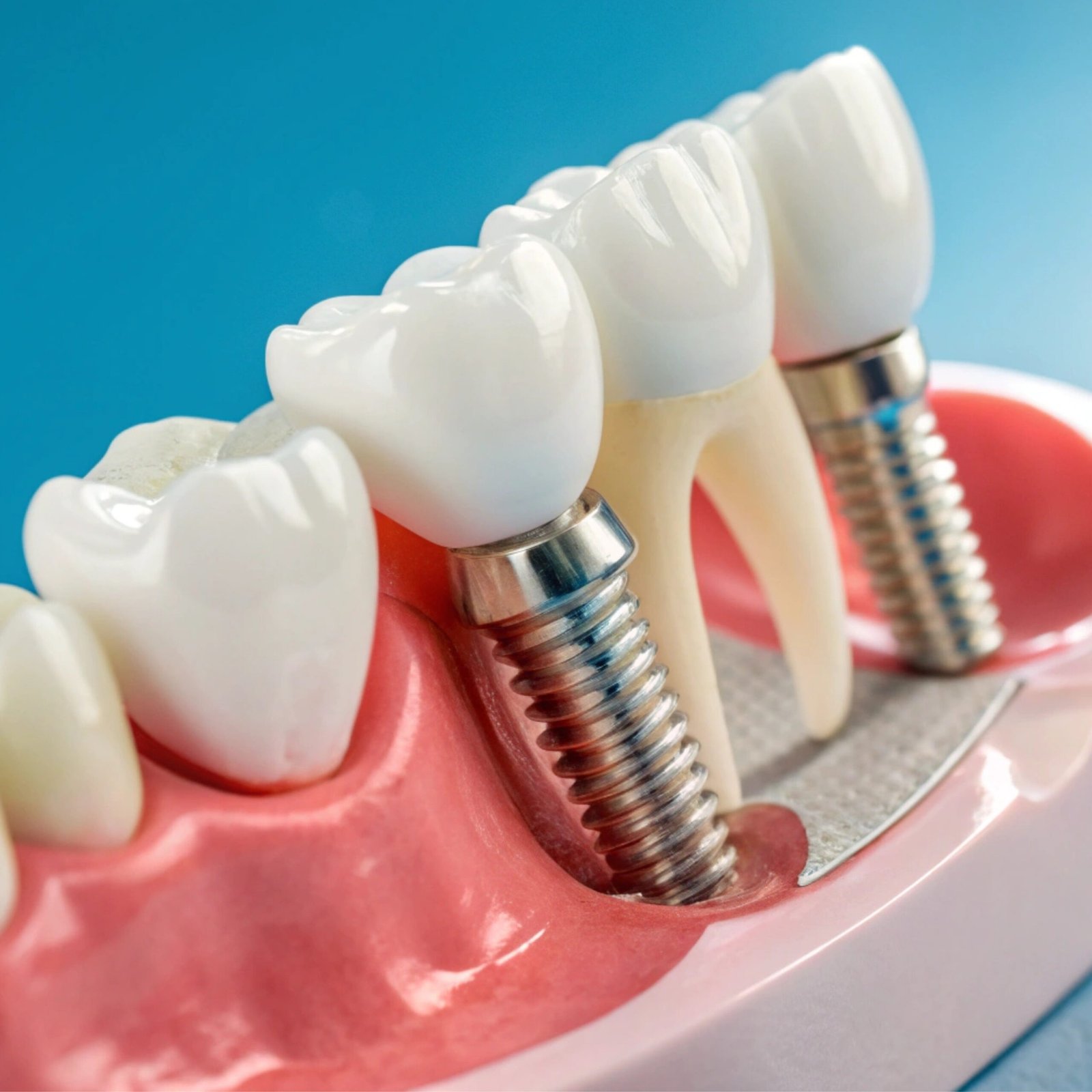
Why is Missing Teeth Important?
Tooth loss is not just an aesthetic problem; it can have an impact on chewing function, speech, jaw joint health and even diet. Even the loss of a single tooth can, over time, cause neighboring teeth to fall into the gap, the tooth in the opposite jaw to elongate and chewing forces to be unevenly distributed. This can create a chain of events that can lead to tooth wear, jaw joint disorders and digestive problems.
When more than one tooth is missing, the load distribution is further distorted; the remaining teeth begin to carry more load than normal. This can lead to faster wear and tear of the remaining teeth over time. In terms of aesthetics, tooth loss, especially in the anterior regions, can cause avoidance of smiling, withdrawal in social environments and loss of self-confidence.
Tooth loss can be treated with different approaches such as traditional bridges, removable prostheses or dental implants. The dentist decides which method is appropriate, taking into account the number of missing teeth, the amount of bone, the condition of neighboring teeth, the general health status and expectations of the patient.
Jawbone, Implant and Osseointegration Process
One of the most important factors in the long-term success of dental implants is the quantity and quality of the jawbone in which the implant is placed. After tooth extraction, the bone in the relevant area may lose volume over time; this process is called “resorption”. Therefore, restorative solutions planned immediately after tooth extraction or within a reasonable period of time may gain importance in terms of reducing bone loss.
Once the implant is in place, instead of rejecting it as a foreign body, the body is able to form new bone tissue around it thanks to the biocompatible nature of titanium. This process osseointegration called osseointegration. Osseointegration time can usually vary from a few weeks to several months, depending on factors such as the implant surface technology used, bone density, the patient's systemic health and oral hygiene.
In some cases, bone augmentation (grafting) is considered when the volume of the jawbone is insufficient. The decision as to when bone augmentation is necessary, the type of material used and the healing time can only be made by the dentist and, if necessary, related specialists after a detailed examination and imaging.
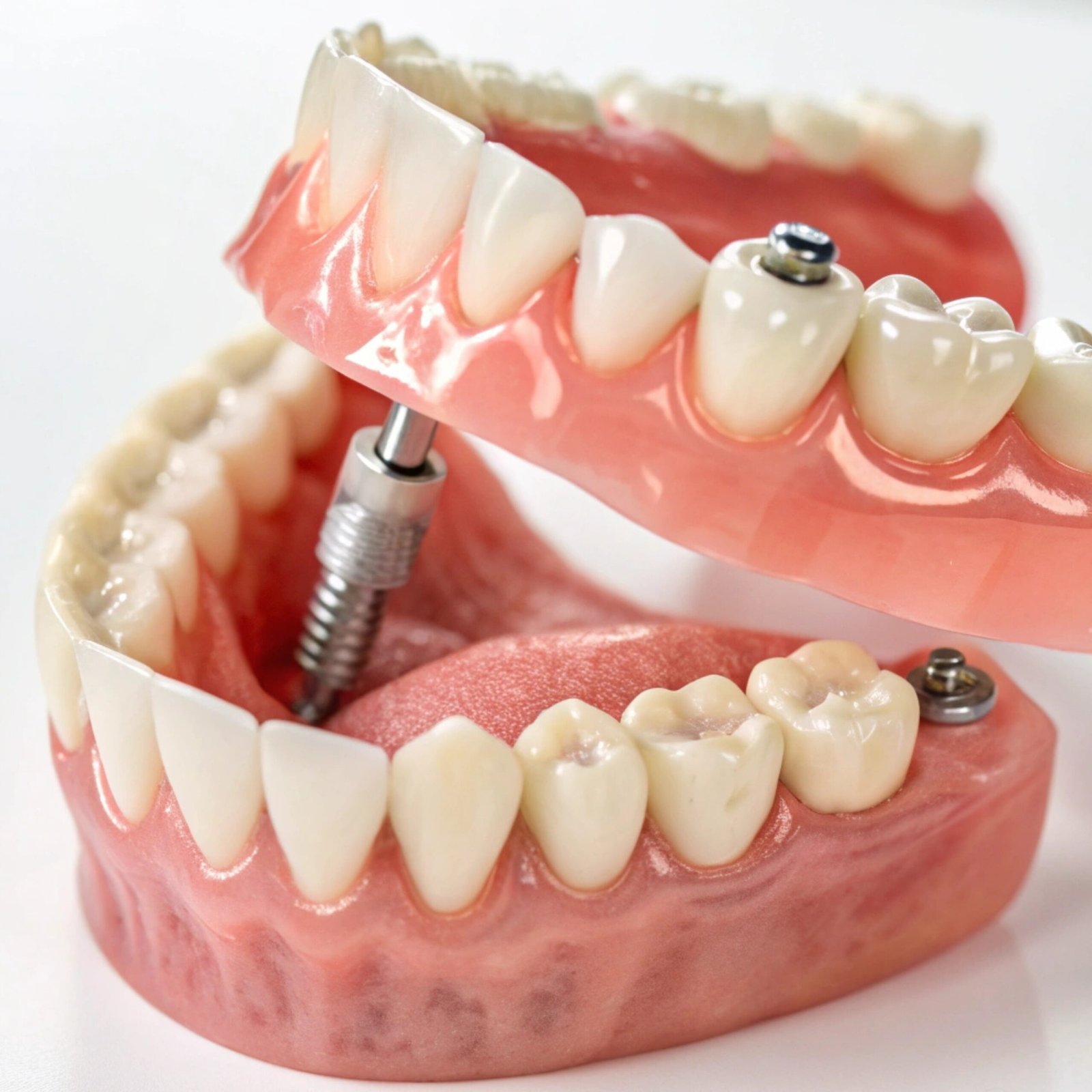
Which Stages Does Implant Treatment Consist of?
Implant treatment is a planned process, often consisting of several stages. The duration of the treatment may vary depending on the number of implants required, bone condition, additional surgical requirements and the general health of the patient. In general terms, the process may consist of the following stages:
1. Examination, Radiographic Examination and Planning
In the first stage, the dentist performs a detailed intraoral examination to assess the condition of the existing teeth, gums, chewing relationship and bite. Bone height and thickness are analyzed, usually using methods such as panoramic x-rays and in some cases 3D imaging (CBCT). This data is important for the number, diameter, size and position of the implant.
2. Preparatory Treatments if necessary
If there are widespread caries, active gum infections, advanced calculus or chronic inflammatory foci in the mouth, it is recommended to address these problems before the implant. This creates a healthier environment for the surgical procedure and supports the chances of long-term success. In some cases, teeth that need to be extracted are evaluated together with implant planning.
3. Placement of the Implant in the Jawbone (Surgical Phase)
Under appropriate local anesthesia, a socket is surgically prepared in the area where the implant will be positioned and the implant is placed in this socket. In some cases, a temporary closure screw or healing cap may be used in the same session as the implant. The duration of the surgical phase may be relatively shorter in single implant applications, but may take longer in cases where more than one implant is required.
4. Healing and Osseointegration Process
After the implant is placed, a certain healing time is expected for the fusion between the bone and the implant surface to take place. This time may vary depending on the jaw region (upper/lower jaw), bone density and the systems used. In some cases, superstructure planning can be done in a shorter time with controlled loading protocols, while others may require longer waiting times. The length of this period is determined by the dentist based on the patient's individual situation.
5. Superstructure (Prosthesis) Phase
After the implant is fused with the bone, the prosthesis to be placed on the implant is started. For this, first the location of the implant in the mouth is revealed with special caps, then the laboratory process is started by taking impressions. Single tooth crowns, bridges or implant-supported prostheses are planned at this stage. The superstructure material and design to be used are determined according to factors such as chewing forces, aesthetic expectations and compatibility with other teeth.
6. Controls and Long Term Follow-up
Implant treatment is not completely “finished” with the delivery of the prosthesis. To maintain long-term success, it is important to go for regular check-ups, have professional scaling (if necessary) and follow the hygiene habits recommended by the dentist. In this way, both the gum tissue around the implant and the fit of the prosthesis can be monitored.
For whom can implant treatment be considered and for whom can it be limited?
Implant treatment is not a standardized procedure to be routinely applied to every person with missing teeth. The assessment of suitability is individualized for each patient. While the information provided below provides a general framework, the final decision can only be made after a dental examination and, if necessary, in cooperation with the relevant medical specialties.
Examples of situations where implant treatment may be considered:
- Individuals who have a single tooth deficiency and do not want their neighboring teeth to be cut
- Cases with multiple missing teeth and insufficient support with a conventional bridge
- In case of complete edentulism, patients who have problems with their removable prostheses and have appropriate bone structure
- Some complex cases where additional support is needed to make masticatory function more stable
Examples of situations that may require caution and limitations in implant treatment:
- Uncontrolled diabetes
- Serious cardiovascular diseases and use of blood thinners (may require consultation between physicians)
- Diseases affecting the immune system or use of medication
- Heavy smoking
- Very severe bone loss (in some cases bone augmentation procedures may be considered)
- Elective surgical procedures can often be postponed during pregnancy
These headings are only general examples; they are not the sole reference for the decision to implant or not. The dentist's assessment is based on personal medical history, medications and radiologic findings.
Implant Supported Solutions for Single Tooth, Multiple Teeth and Complete Edentulism
Implants can be evaluated in different scenarios, ranging from single missing teeth to multiple missing teeth and cases where all teeth are missing. The number of implants to be used and the superstructure design are planned together by the dentist and the relevant specialists.
1. Implant Supported Crown in Single Tooth Deficiency
Especially in cases of single tooth loss in the anterior region, implant-supported single tooth crowns can be considered for people who do not prefer to cut neighboring healthy teeth for bridges. The implant is placed in place of the missing tooth and a crown is designed to mimic the form of that tooth. Neighboring teeth can be left in place with a more protective approach. However, the suitability of this treatment depends on the width of the gap, bone volume and the condition of the adjacent teeth.
2. Implant Supported Bridges in Multiple Tooth Loss
In cases where two or more teeth are missing, instead of placing implants for each gap individually, bridges can be planned on implants placed at certain intervals. For example, a gap of three teeth can be solved with two implants and a body tooth in between. This planning is done by taking into account the balanced distribution of chewing forces, the density of the bone and the design of the prosthesis.
3. Implant Supported Prostheses in Complete Edentulism
In cases where there are no teeth in the upper or lower jaw, conventional total dentures may not be mobile, movable or adequately retained in some patients. Under favorable bone conditions, fixed bridge prostheses using a certain number of implants or removable prostheses supported by implant retainers can be planned. In this way, the retention of the prosthesis can be increased. The number of implants and the type of prosthesis to be used are evaluated by the dentist according to the patient's oral structure, bone condition and expectations.
4. Implant-Mounted Removable Prostheses (Overdenture Systems)
In some cases of complete edentulism, instead of a completely fixed bridge, removable prostheses supported by several implants and retainers attached to them may be considered. These systems can provide more retention than conventional total dentures and allow the user to remove and clean the prosthesis when necessary. Which system is more appropriate is determined after clinical examination and radiologic evaluation.
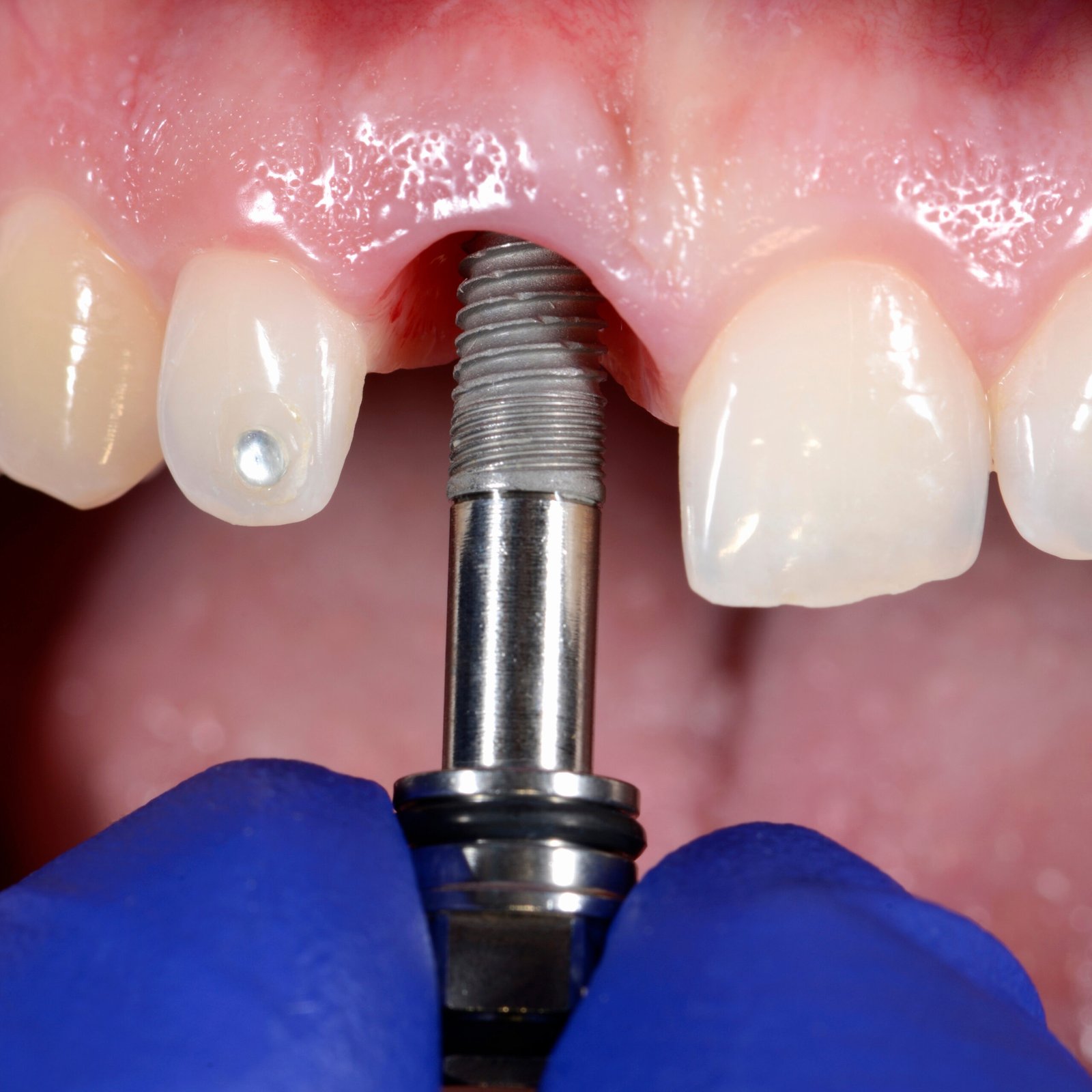
Post Implant Care, Oral Hygiene and Long Term Follow-up
Post-treatment care plays as important a role in the success of implant treatment as the surgical and prosthetic phases. Keeping the gum and bone tissue around the implant healthy is closely linked to regular oral hygiene and professional check-ups. As with natural teeth, bacterial plaque can accumulate around the implant, which can build up over time. peri-implant mucositis and peri-implantitis can lead to inflammatory problems such as.
Oral care recommendations for the peri-implant area (general information):
- Brushing the teeth and around the implant prosthesis with soft bristled brushes at least twice a day
- Using interdental brushes, dental floss or special cleaners recommended by the dentist
- Quit or reduce smoking if possible (important for tissue healing and long-term success)
- Attending professional cleaning and check-up appointments at the intervals recommended by the physician
- Notify the physician without delay in case of an abnormal sound, pain, sensation of movement or suspicion of fracture during chewing
During physician controls; the color of the gum around the implant, bleeding status, pocket depths, screws or fasteners of the prostheses can be examined. Thus, problems can be detected at an early stage before they grow.
General Information About Possible Problems After Implant Treatment
As with all surgical and prosthetic procedures, implant treatment has its own risks and potential complications. The following information provides a general framework and should not be considered as a direct prediction for individual patients.
- Pain and tenderness in the first days: Mild to moderate pain and tenderness may be observed for a few days after the surgical procedure. This condition can usually be controlled with painkillers recommended by the physician.
- Swelling and bruising: Especially with multiple implants and additional surgical procedures, there may be swelling and bruising that may last for several days.
- Discomfort at the suture site: There may be a slight stinging or pulling sensation in the area until the stitches are removed.
- Failure of the implant to fuse (failure of osseointegration): In rare cases, the implant may not fuse with the bone as expected. In this case, the treatment process may continue with different steps, such as implant removal or replanning.
- Peri-implant inflammation: Without regular care, inflammation and bone loss may develop around the implant. If recognized at an early stage, it can be controlled with the necessary treatments.
- Mechanical problems with the prosthesis: Over time, loosening of the prosthetic screw, wear of the fasteners or porcelain fractures may occur. These situations can usually be resolved by repair or replanning.
The assessment of possible risks and complications is considered together with the patient's systemic condition, bone structure and habits (smoking, oral care, etc.). When any suspicious symptoms occur, it is important to contact the dentist instead of seeking a solution on your own.